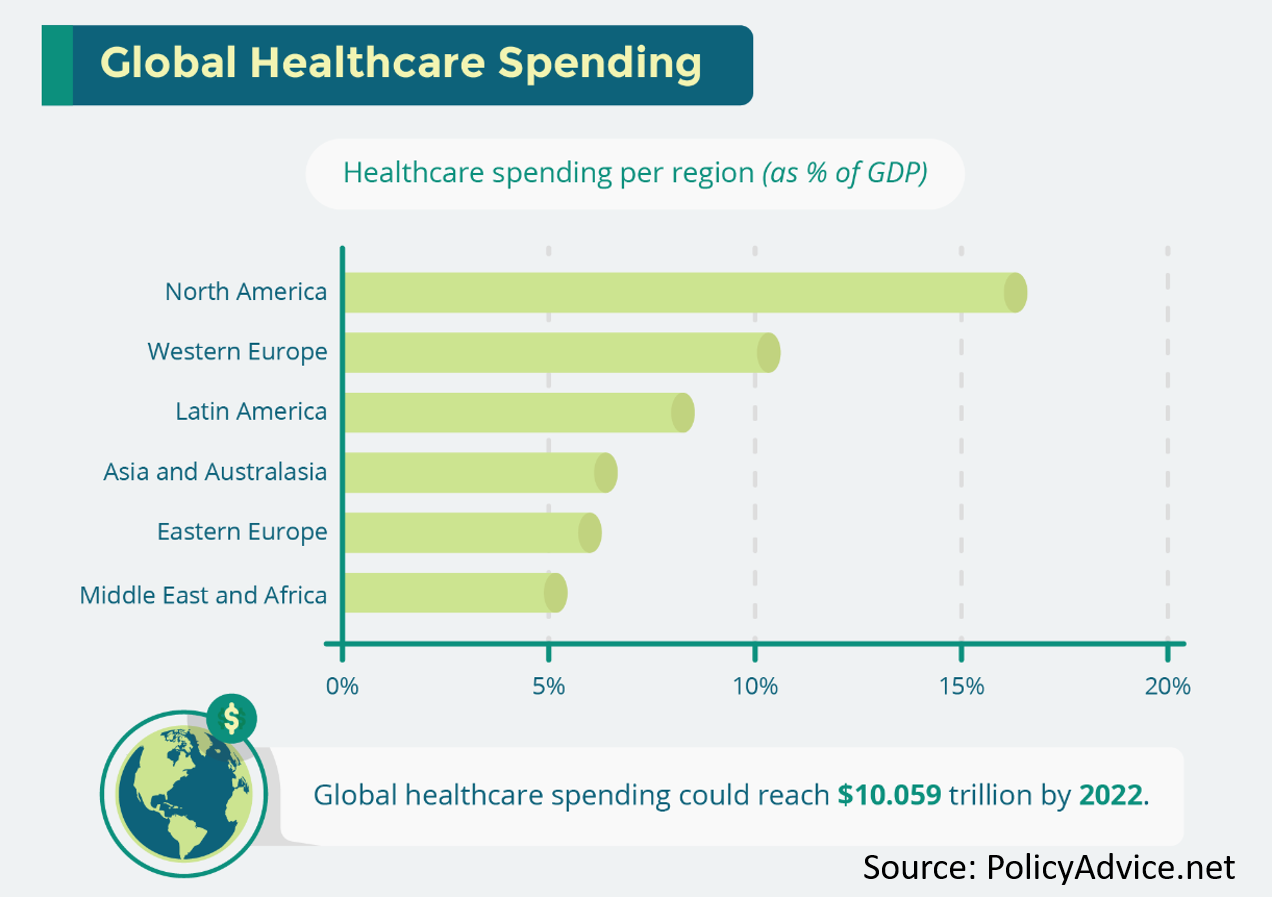
While the US boasts some of the most distinguished healthcare institutions and experts in the world, it is no match for the health and economic destruction of COVID-19. Worse, it has exposed weaknesses in a US health system that is large and complex. According to PolicyAdvice.net the US spends over $10,000 per capita on healthcare, twice the rate of other developed countries, yet it is struggling to provide care systematically to those in need, whether COVID-19-related or not. “This crisis has lifted the veil on the vulnerability we have as a healthcare system,” says Ann Garnier, CEO of Lisa Health, a San Francisco-based healthcare startup focused on middle-aged women’s wellbeing.
The Social Impact Advisory Group for its Social Impact Speaker Series asked industry experts about some of the vulnerabilities and how best to tackle them. Access to healthcare was the overarching theme.
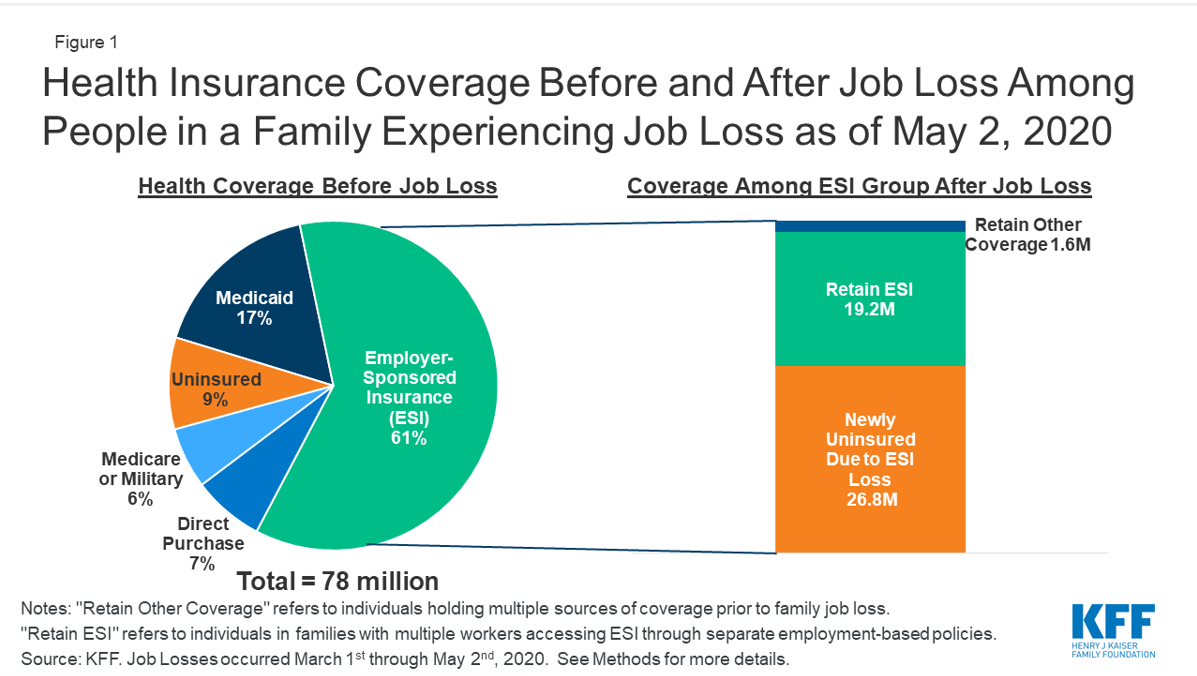
About half of the US population relied on employer-sponsored health insurance before the coronavirus crisis. Now with millions unemployed and nearly one million Americans applying for unemployment benefits, the Kaiser Family Foundation estimates that nearly 27 million people have lost healthcare coverage. Unlike residents in other developed countries, these unemployed Americans cannot rely on a national healthcare system and instead must navigate a patchwork safety net of programs. While many of the unemployed will be eligible for Medicaid or Affordable Care Act credits, there is still a large number of Americans who will be eligible for neither. “We’re having a lot of big conversations around what the role of an employer is in terms of their employees and the larger community,” says Emily London, Senior Manager at the Pacific Business Group on Health, a nonprofit collaborative of the largest private and public purchasers of healthcare.
Before the crisis, the topic of a national healthcare system that would cover all Americans was controversial and enjoyed little support if it meant eliminating private insurance. With the virus still raging, universal healthcare may be gaining support. “We have two unique opportunities which could accelerate the move toward universal coverage. First, an appreciation for public health infrastructure that we didn’t have before the crisis. And second, universal primary care…that would be a significant shift in both access and prevention and delivery of care,” says Jim Hickman of Hickman Strategies, a communications and resource mobilization consultancy based in Oakland, CA. In other words, by providing all Americans with healthcare that focuses on the whole individual rather than specific illnesses, the US can improve overall public health.
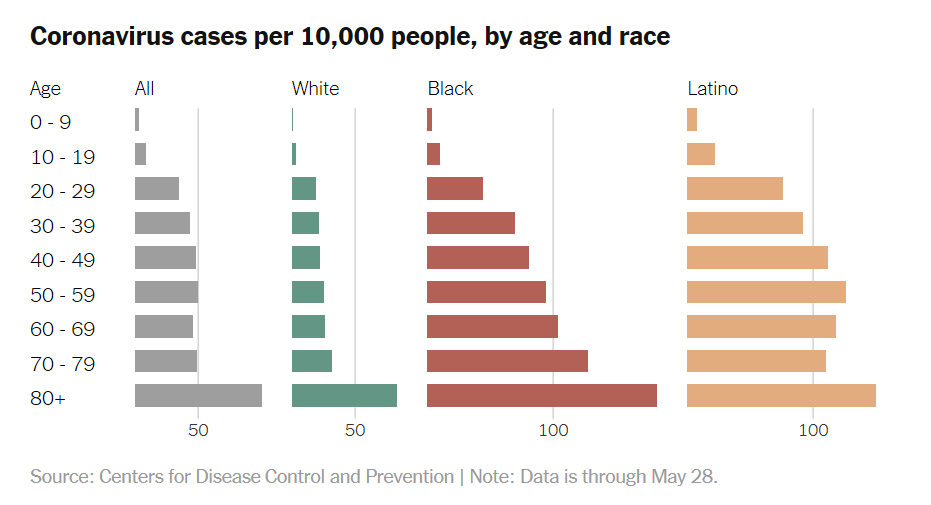
While employment has rebounded significantly with many furloughed employees returning to work, front line workers are often in jobs that provide inadequate healthcare coverage through their employer-sponsored plan. Namely new federal data shows that African-Americans and LatinX people, who make up a disproportionate amount of those returning to work, are three times more likely to contract the virus and two times more likely to die from the virus, according to data made available to the New York Times after suing the CDC. In addition, COVID-19 is seriously affecting people with highly treatable diseases like hypertension and diabetes. Better access to primary care for these at-risk communities might have reduced the threat of the contagion
Dr. Eleanor Britter, a retired physician, provides free healthcare to all who need it through the Peninsula Special Interest Lions Club Charities clinic to demonstrate the value of universal healthcare. “We need to show them and prove to them that this is necessary…It’s a matter of getting it emotionally in their gut that we need this kind of socialized medicine.” The current crisis seems to be indeed changing opinions as voters in Oklahoma just approved Medicaid expansion since the onset of COVID-19. Voters in Missouri will also be allowed to vote on Medicaid expansion in August.
If there has been one silver lining to this crisis, it has been the expansion of technology in delivering healthcare, with a particular focus on telemedicine.
Telemedicine has been around for decades, yet providers were reluctant to use the service due to high technology costs, poor understanding of the platform and, more importantly, insurance coverage restrictions. The CARES Act has loosened restrictions on virtual office visits to allow patients to stay at home during the COVID-19 pandemic, but it has also brought other benefits of telemedicine, such as reduced cost, reduced hospitalizations and increased patient compliance. Telemedicine has also proven to be an effective and convenient means to treat chronic illnesses such as hypertension, diabetes and lung disease.
COVID-19 may force the US health care system to make foundational changes thyat increase access and lower costs. “We’re finally learning as an industry that we need to innovate at a pace that’s more akin to other industries and it’s OK to move more quickly. COVID has forced providers to adapt,” says Lisa Health’s Ann Garnier.
Talk to the financial experts at Fairlight Advisors to learn more about managing your nonprofit’s investments. Schedule a free consultation today!
Fairlight Advisors
Latest posts by Fairlight Advisors (see all)
- Market & Economic Snapshot Q1 2026 - April 29, 2026



